Surgery
Outpatient operations offered in our offices
In our offices, I offer surgical procedures that are conducted using local anesthetic This includes, for example, male sterilization (vasectomy), the removal of skin alterations, nodes, tumors or ingrown nails on an outpatient basis and with local anesthetic. I have acquired great experience in the area of outpatient liposuctions This is the perfect method for permanent removal of unwanted fat deposits.
The majority of outpatient hand surgeries are conducted with a regional anesthetic. Examples include: trigger finger, tendinitis, nerve compression disorders (e.g. carpal tunnel syndrome) or ganglia).
Anesthetics used in our offices
For a local anesthesia the operative area is injected with a solution containing an anesthetic (e.g. xylocaine) and is thus made insensitive. This solution has an added vaso-constrictive agent (adrenaline) which leads to less bleeding and an increased duration of the insensitivity. With anesthetics in the fingers, toes, ears, or nose the circulation is not affected, so vaso-constrictive agents are not used in these places.
For hand surgeries we often use regional anesthetic methods: the upper part of the affected arm is covered with a double cuff, much like a blood pressure cuff. A fine cannula (Venflon) is inserted into the arm vein. The extremity in question is then raised and then “wrapped” from front to back with a bandage thus achieving a state of bloodlessness that simplifies the operation. Finally the cuff that is closer to the body is put under pressure. Now the anesthetic agent (Ivracaine 0.5%) is injected into the previously inserted plastic cannula, which distributes over the entire arm up to the cuff. After about 10 minutes, the pressure between the two cuffs is retroverted. Here the tissue has in the meantime become insensitive as a result of the anesthetic, and thus the cuff pressure can be maintained without a problem for up to around an hour. After releasing the cuff pressure, full sensitivity returns after about 10 minutes. During regional anesthesia, blood pressure, pulse, oxygen saturation of the blood and the heart rate are continuously monitored, and for larger procedures and with older patients, an infusion is used.
Before the operation

In general, we make a first appointment prior to the procedure to get to know you personally and for an examination. This is important, so that you are informed about the outcome, the follow-up care, the risk and the potential incapacity to work as a result of the planned operation. Besides the conversation with the patient, for me this is also about planning the procedure while considering the personnel requirements, the instruments, and the time needed. For smaller procedures with an unequivocal diagnosis (e.g. with referral from your family physician) and if everything is clear for you, then the operation can be done directly and without preliminary discussion.
Outpatient procedures require the reliable cooperation of the patient. Thus it is important that you observe the following guidelines.
Please pay attention to cleanliness: thoroughly clean the areas designated for the operation with soap. For procedures on the hands or feet, the nails should be trimmed and clean. Remove all nail polish. For procedures on the hand or arm, jewelry or rings should be removed, and similarly no earrings should be worn for procedures in the area of the ear. Wear suitable clothing (e.g. well-fitting shoes for operations in the foot area, a sweatshirt with loose sleeves for procedures on the arm or hand).
Depending on the procedure, please organize transportation home in advance (e.g. an acquaintance with a vehicle). Please consider that at home, you will not always be able to perform your usual activities, depending on the type and size of your operation. Thus, organize your work in advance if possible, or get someone to help you around the house.
After the operation

You should pay attention to a few things after the operation. The operation wound site should be protected and left alone. You should absolutely avoid heavy or dirty activities. The affected part of the body should be elevated when possible (e.g. wear an arm sling or elevate your legs). Thus swelling is reduced and you will need less or even no pain medication. In addition, this helps speed up the healing process of the wound. In the first 2-3 days, it would also help to cool the wound (e.g. by applying towel-wrapped cold packs for 20 minutes at a time, several times a day).
As pain medication in reserve, we give you either Aulin (maximum of 2-3 x 100mg sachets per day), Dafalgan (maximum of 8 500mg tablets per day), Ponstan (maximum of 3 x 500mg tablets) or Panadol (maximum 8 500mg tablets per day)..
In cases of intense pain, if there is bleeding through the dressing, or in the event of fever or chills, or “formication” after surgery on the arms or legs, please call our offices (+41 -32 636 25 25).
The follow-up after a procedure and the removal of stitches takes places either with us or in the office of your family physician. Of course, we are always available for questions or problems in the first few days after an operation even outside of office hours (cell phone +41 -79 215 86 86).
Scars—what can be done about them?
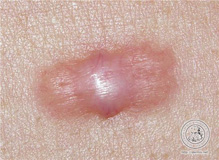
The formation of scars varies greatly from person to person and depends on your personal healing tendencies. A number of external factors such as age, damaged wound edges (bruised or burned), unfavorable location (near a joint or in the décolleté area), dark skin type, or illnesses such as circulation disorders, diabetes or excessive smoking can negatively affect the formation of scars.
Your wounds are closed with the finest suture material and tissue-protecting technique; for ideal scar generation, you can also make essential personal contributions. Stretching forces should be avoided. Sutured wounds are under tensile pressure, particularly after removal of tissue. This tension pulls the scars. Ideal, line-shaped scars thus often require strain relief by fine adhesive patches (Steri-Strips) stretched across the wound.
Every scar goes through an inflammatory stage with swelling and redness, that peaks at around 4 weeks and slowly disappears on its own again. At the same time, the scar can become knotty, hard and elevated. At this point, the scars should be massaged flat with pressure several times a day. Special scar ointments assist in this pressure massage. In stubborn cases (e.g. after burning or with a predisposition to excessive scarring), the scars must be covered with a silicone layer (e.g. Silastic Gel or Mepiform) for a while. Only seldom is it necessary to wear a custom-fitted pressure suit, which provides a long-term and even pressure on the scars. Sunlight or tanning beds enable fresh scars to remain darkly pigmented. The scars must therefore be covered as long as they are still reddish (a bandage or total sunblock).
The healing of the scars takes several months, so have patience. Scars at tension points, over joints, or from burns take at least a year to become pale and soften. During this time the annoying itching and sometimes unusual sensations in the scar area will disappear as well.

